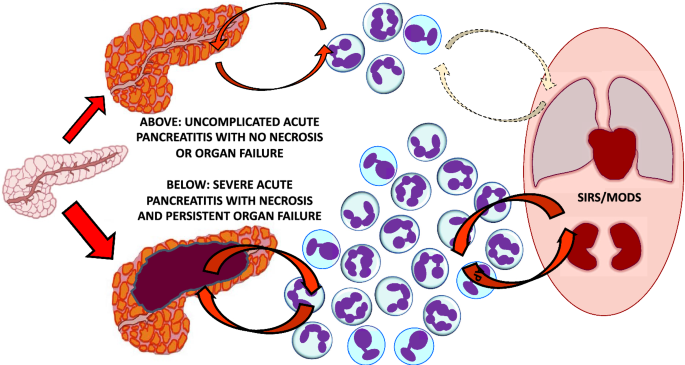
Acute pancreatitis is a common digestive system disease with rapid onset and rapid progression, posing a serious threat to the patient's life and health. This article will comprehensively discuss acute pancreatitis from four aspects: medicine, clinical trials, epidemiology and medical care.
In medicine, the causes of acute pancreatitis are diverse, including biliary tract disease, alcoholism, hyperlipidemia, etc. These causes cause pancreatic enzymes to be activated in the pancreas, triggering autodigestion of pancreatic tissue, leading to pancreatic inflammation and necrosis. Typical clinical manifestations of acute pancreatitis include abdominal pain, nausea, vomiting, fever, etc. In severe cases, shock and multiple organ failure may occur. Diagnosing acute pancreatitis usually requires blood and urine amylase tests, abdominal ultrasound, CT and other imaging tests to confirm the condition. The treatment of acute pancreatitis mainly includes fasting, gastrointestinal decompression, anti-inflammation, inhibition of pancreatic enzyme secretion and other measures to reduce the patient's pain and control the progression of the disease.
In terms of clinical trials, many studies are devoted to exploring treatments for acute pancreatitis. A randomized controlled trial compared the effect of early surgery with conservative treatment in acute pancreatitis. The results showed that the mortality rate of patients in the early surgery group was higher than that in the conservative treatment group. Therefore, early surgery is not the first choice treatment for acute pancreatitis. In addition, clinical trials have also focused on the role of traditional Chinese medicine in treating acute pancreatitis. A double-blind randomized controlled trial showed that the traditional Chinese medicine group was significantly better than the control group in improving clinical symptoms and reducing amylase levels, suggesting that traditional Chinese medicine has potential application value in the treatment of acute pancreatitis.
In terms of epidemiology, the incidence of acute pancreatitis is on the rise, and its incidence is related to lifestyle, dietary structure and other factors. Alcoholism, hyperlipidemia, and biliary tract disease are the main risk factors for acute pancreatitis. In addition, epidemiological studies have found that the mortality rate of acute pancreatitis varies by region and population, and the overall mortality rate is high, placing a heavy burden on society and families.
In terms of medical care, measures to prevent acute pancreatitis include improving lifestyle, eating a reasonable diet, controlling blood lipids, etc. For patients with acute pancreatitis, timely diagnosis and treatment are crucial. Home care, rest, and diet are important in treating and preventing acute pancreatitis. Patients should follow medical advice, arrange their diet reasonably, avoid high-fat and high-protein foods, and pay attention to rest to avoid overexertion.
In short, acute pancreatitis is a serious digestive system disease, and a deeper understanding of it can help improve diagnosis and treatment and improve patients' quality of life. Future research can focus on the pathogenesis of acute pancreatitis, the exploration and clinical application of new treatment methods, and at the same time strengthen epidemiological investigations to provide more basis for the prevention and treatment of acute pancreatitis. As medical staff and patients, we should pay attention to the medical knowledge of acute pancreatitis and adopt a healthy lifestyle to reduce the risk of disease and improve treatment effects.
Recurrent Acute Pancreatitis in the Setting of Abnormal Pancreaticobiliary Junction